Reminder: Data Validation Tool Instructions
BCBSWY updated our Directory Validation tool instructions on the Availity Portal. The instructions include directions for Providers to find NPI and tax ID combinations to help facilitate compliance with the No Surprises Act (NSA) provider directory validation requirements. The NSA requires you confirm this information with us every 90 days, so your information can continue to be listed in our public directory. Please see the updated guide here.
Sign up to Receive New and Improved Provider Update
The BCBSWY Provider Update Newsletter is getting a makeover. Please sign up at BCBSWY.com to continue receiving these updates with a fresh new look. Please note: Only those who have signed up since December 1, 2021 will be carried forward.
Authorization Pre-Check Tip
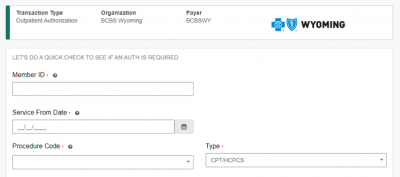
The Authorization Pre-Check tool allows you to determine if a prior authorization is required for a member upfront. Simply enter the requested information below and you will get a yes or no answer if an authorization is required. Keep in mind, this is for BCBSWY members only. For other Blues plans and FEP click “Skip” at the bottom of the page. Keep an eye out for more details!